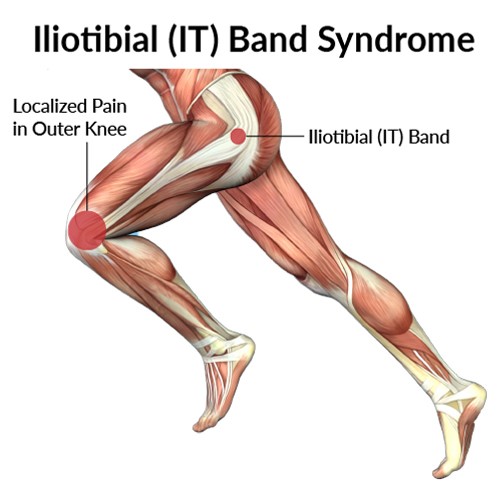
If you’re an athlete experiencing aching or sharp pain on the outside of your knee or hip, you might have a tight iliotibial band. Your iliotibial band is a tendon that can rub against your hip or knee bones. The swelling and irritation can cause several symptoms. You might need physical therapy, medications or, rarely, surgery.
Iliotibial band syndrome is where a tendon called the iliotibial band gets irritated or swollen from rubbing against your hip or knee bones. The tendon is on the outside of your leg, and it goes from the top of your pelvic bone down to your knee. It rubs against your bones when it gets too tense (tight). There are many reasons why your iliotibial band might tighten.
Tendons are flexible, elastic-like fibrous tissues that connect your muscles to your bones. Your tendon pulls on the bone when you squeeze a muscle, and that makes your bone move.
You can have iliotibial band syndrome in one leg, or you can have it in both legs. When you have ITBS in both legs, it’s called bilateral iliotibial band syndrome.
You’re at a higher risk for iliotibial band syndrome if you’re young and exercise frequently. Examples of athletes who are most prone to ITBS include:
Even if you’re not an athlete, there are still some traits that give you a slightly above average chance of getting iliotibial band syndrome. Reasons include:
Experts note that iliotibial band syndrome often affects U.S. Marines during training. More than 20% get iliotibial band syndrome. Frequent runners, especially long-distance runners, are also prone. Iliotibial band syndrome accounts for about 12% of running injuries. More females than males have iliotibial band syndrome.
Knee pain — of which iliotibial band syndrome is one of many causes — affects as many as 25% of adults.
Your iliotibial band gets irritated and swollen when it’s stretched too tight and rubs against bone. Possible causes of a tight iliotibial band include:
Your tight iliotibial band might rub against your bones for reasons that include:
A tense iliotibial band can cause several symptoms:
At first, the pain will start after you exercise. As the syndrome worsens, you’ll feel it the whole time you exercise and, eventually, also when you’re resting.
This method is similar to the Ponseti method, but it uses splinting and taping instead of casting. A splint is a device that supports and protects bones.
A physical therapist performs this treatment. They’ll start the treatment soon after birth. This treatment needs to be done every day rather than once a week. But you don’t need to return to the physical therapist each time. The physical therapist sees your child a few times a week and teaches you how to do the splinting and taping at home.
How to do the French method to fix clubfoot:
There are several types of braces. Your provider will discuss your options so you can find the right brace for your child.
Sometimes, a child has severe clubfoot. Or you’ve tried nonsurgical methods, but they haven’t worked. Surgery can correct the problem. It’s best if your child has the surgery before they start walking. During the procedure, the surgeon:
A few weeks after the surgery, the surgeon:
There’s still a chance their foot could return to the clubfoot position. Your provider may recommend bracing or special shoes to keep their foot in the correct position.
Risks of congenital clubfoot surgery include:
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec