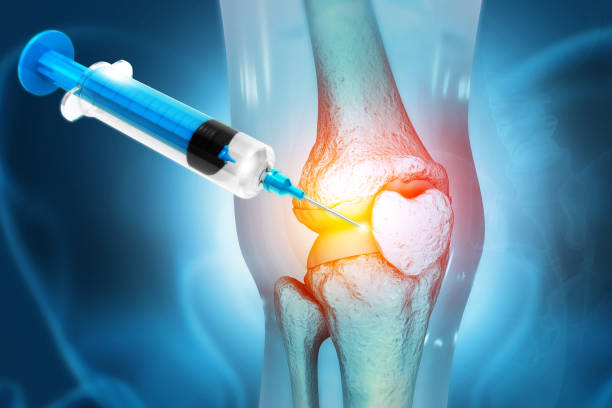
Joint aspiration, also known as arthrocentesis, is a medical procedure that involves the removal of fluid from a joint using a needle and syringe. This technique is both diagnostic and therapeutic, playing a crucial role in the management of various joint disorders. By extracting synovial fluid, healthcare providers can analyze it to diagnose infections, inflammatory conditions, or crystal-induced arthritis, and also relieve joint swelling and pain. Understanding joint aspiration is important for patients and clinicians alike, as it aids in timely diagnosis and effective treatment of joint-related ailments.
Joints are the connections between bones that allow movement and provide mechanical support. Most joints are synovial joints, characterized by a joint capsule lined with synovial membrane that produces synovial fluid. This fluid lubricates the joint, reduces friction, and nourishes the cartilage. Commonly aspirated joints include the knee, shoulder, elbow, wrist, ankle, and hip.
The synovial fluid resides within the joint cavity, surrounded by the joint capsule and supported by ligaments and tendons. In pathological conditions, excess fluid (effusion) can accumulate, causing swelling and pain. Arthrocentesis targets this fluid to obtain samples for laboratory analysis or to reduce pressure within the joint.
Joint aspiration is typically performed when there is an abnormal accumulation of fluid in the joint, which can be caused by:
Risk factors include a history of joint injury, immunosuppression, existing joint disease, or recent infections.
Patients requiring joint aspiration often present with:
The severity and combination of symptoms depend on the underlying cause.
Diagnosis involves a combination of clinical evaluation and investigations:
Treatment depends on the underlying cause identified through aspiration:
Non-surgical:
Surgical:
The joint aspiration procedure typically involves the following steps:
The procedure usually takes a few minutes and is performed in an outpatient setting.
After joint aspiration:
Though generally safe, joint aspiration carries some risks:
Proper technique and sterile conditions minimize these risks.
The prognosis after joint aspiration depends on the underlying condition:
Early diagnosis and treatment improve outcomes significantly.
Seek medical attention if you experience:
Timely evaluation can prevent complications and preserve joint function.
Joint aspiration (arthrocentesis) is a vital procedure for diagnosing and managing joint disorders. By understanding its purpose, procedure, and associated care, patients can better appreciate its role in relieving symptoms and guiding treatment. If you experience joint swelling, pain, or other related symptoms, consult a healthcare professional promptly to determine if joint aspiration is appropriate for your condition. Early intervention can lead to improved outcomes and enhanced quality of life.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec