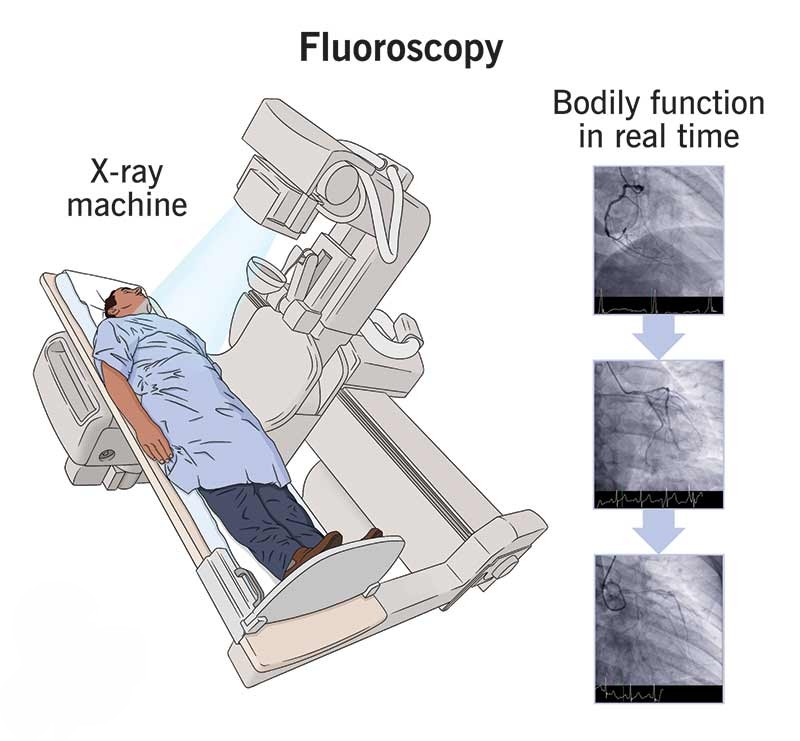
Fluoroscopy is a medical imaging technique that provides real-time moving images of the internal structures of the body using X-rays. Unlike static X-ray images, fluoroscopy allows physicians to observe dynamic processes such as the movement of joints, the flow of contrast agents through blood vessels, or the function of the gastrointestinal tract. This capability makes fluoroscopy an invaluable tool in diagnosis, treatment planning, and guiding minimally invasive procedures.
The importance of fluoroscopy lies in its ability to offer continuous visualization, which enhances the accuracy of interventions and improves patient outcomes. It is widely used in various medical specialties including orthopedics, cardiology, gastroenterology, and interventional radiology.
Understanding fluoroscopy requires a basic knowledge of the anatomical regions commonly examined with this technique. For example:
The diagnostic process involving fluoroscopy includes:
The real-time imaging allows clinicians to observe physiological processes and make accurate diagnoses.
Fluoroscopy is not a treatment but a diagnostic and procedural aid. However, it plays a crucial role in guiding treatments such as:
The choice of treatment depends on the diagnosis and patient-specific factors.
When fluoroscopy is used for procedural guidance, the steps typically include:
The procedure duration varies depending on the complexity.
Post-procedure care depends on the intervention performed:
Patients are advised to report any unusual symptoms promptly.
While fluoroscopy is generally safe, potential risks include:
Healthcare providers take precautions to minimize these risks.
The prognosis depends on the underlying condition diagnosed or treated with fluoroscopy. Early and accurate diagnosis facilitated by fluoroscopy often leads to better outcomes. Minimally invasive procedures guided by fluoroscopy typically result in shorter recovery times and fewer complications compared to open surgery.
Fluoroscopy is a vital imaging modality that provides dynamic visualization of internal body structures, aiding in diagnosis and guiding a variety of medical procedures. Its ability to offer real-time images enhances the precision of interventions and improves patient care. Understanding the applications, procedure details, and associated risks of fluoroscopy empowers patients and healthcare providers to make informed decisions. If you or a loved one requires fluoroscopic evaluation or treatment, consult with a qualified healthcare professional to ensure safe and effective care.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec