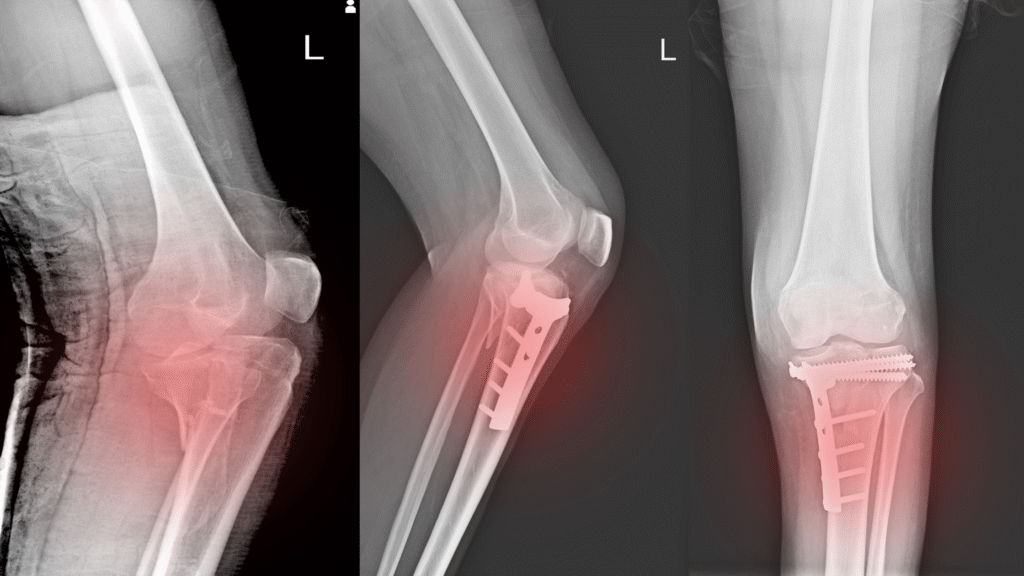
Growth plate fractures, also known as physeal fractures, are injuries that occur in the growth plates of children and adolescents. The growth plate (physis) is a layer of cartilage near the ends of long bones where bone growth occurs. Because these plates are weaker than the surrounding bone and ligaments, they are susceptible to fractures during trauma.
Proper management of growth plate fractures is critical to ensure normal bone growth and to prevent complications such as growth arrest, deformity, or limb length discrepancy. Growth plate fracture fixation is a surgical procedure used to stabilize displaced or unstable fractures of the growth plate, promoting healing and preserving growth potential.
This article provides an in-depth overview of growth plate fractures, indications for fixation, surgical techniques, postoperative care, and outcomes.
The growth plate is composed of cartilage cells that proliferate and ossify to allow longitudinal bone growth. It is located between the metaphysis (shaft end) and the epiphysis (bone end). Because it is the last portion of the bone to ossify, it remains vulnerable to injury during childhood and adolescence.
Clubfoot happens because of an issue with your child’s tendons, the tissues that connect muscle to bone. The tendons in your baby’s leg and foot are shorter and tighter than they should be. That causes the foot to twist. About half of babies with clubfoot have an issue with both feet.
Growth plate fractures are classified by the Salter-Harris system, which helps guide treatment and prognosis:
Types III and IV often require surgical fixation due to involvement of the joint surface and risk of growth disturbance.
Not all growth plate fractures require surgery. Indications for fixation include:
The goal of fixation is to restore anatomical alignment, stabilize the fracture, and minimize damage to the growth plate.
Surgery is performed under general anesthesia. The patient is positioned to allow optimal access to the fracture site.
The choice of fixation depends on the fracture type, size, and location:
Growth plate fractures carry a risk of complications, especially if not properly treated:
The prognosis of growth plate fractures depends on:
With appropriate fixation and care, most children regain full function with minimal long-term issues. However, close monitoring until skeletal maturity is important to identify and address any growth disturbances.
Growth plate fracture fixation is a critical intervention for displaced or unstable physeal fractures in children and adolescents. By restoring anatomical alignment and stabilizing the fracture, this procedure helps preserve the growth potential of the bone and prevents deformities.
Early diagnosis, careful surgical technique, and diligent postoperative follow-up are key to successful outcomes. Parents and caregivers should seek immediate medical attention for suspected growth plate injuries to ensure timely and effective treatment.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec