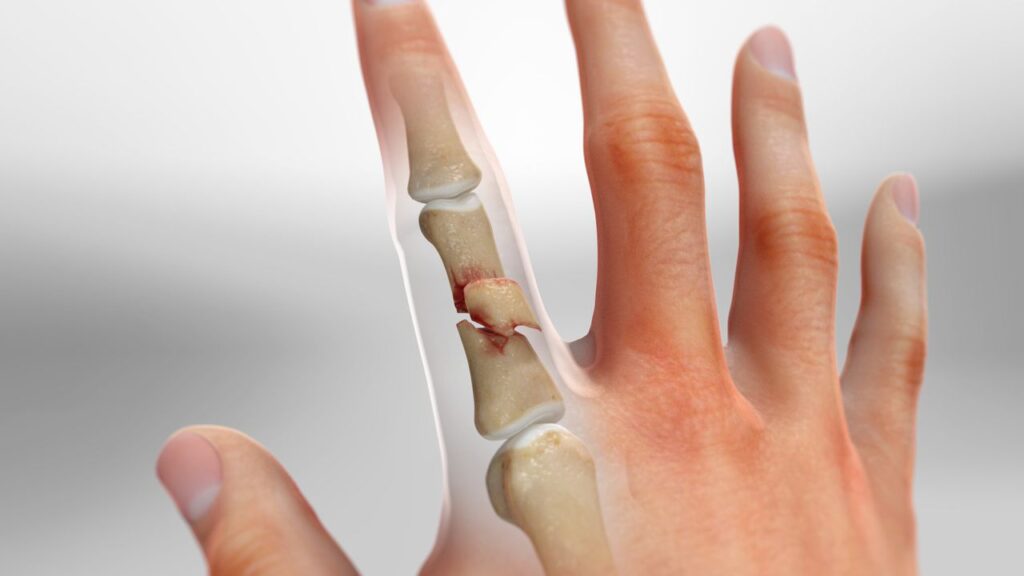
A hand fracture is a break in one of the bones in the hand. This includes:
A broken hand can be caused by a fall, crush injury, or twisting injury, or through direct contact in sports.
In many cases, a hand fracture will heal well with nonsurgical treatment. Depending on the type and location of the fracture, this may include wearing a cast, splint or buddy straps for a period of time. For more serious fractures or for fractures that do not line up properly, however, surgery may be required to realign the broken pieces of bone and keep them in place until they heal.
The bones in your hand include:
The most common hand fracture is a fracture of the fifth metacarpal — the bone in the hand that supports the little finger. This is commonly called a “boxer’s fracture” and involves the “neck” of the bone, next to the knuckle joint. A boxer’s fracture is caused most often by punching or striking a hard object when your hand is closed in a fist. It can also be caused by a fall, motor vehicle accident, or other trauma.
Signs and symptoms of a hand fracture may include:
In the case of a boxer’s fracture, the patient’s knuckle may look sunken in or depressed. This is caused by the displacement or angulation of the end, or “head,” of the metacarpal bone.
Your doctor will ask about your symptoms and perform a careful examination of your fingers and hand. During the exam, they may look for:
Typically, your doctor will evaluate the tendons in your hand to ensure they are functioning properly and will check for instability in the joint(s) near the fracture.
X-rays provide images of dense structures, such as bone. Your doctor may order one or more X-rays to help identify the location and extent of the fracture.
If a fracture does not line up in an acceptable position, your doctor can often realign the bone fragments by gently manipulating them back into position without making an incision. This procedure is called a closed reduction. A cast, splint or brace may be applied to keep the bones in acceptable alignment while they heal. The cast may extend from your fingertips almost to your elbow to support the bones properly.
Your doctor will probably order a second set of X-rays about 1 to 2 weeks later. This is done to ensure that the bones are healing in the proper position.
Depending on the location and stability of the fracture, you may have to wear the cast for 3 to 6 weeks. Some types of fractures can be protected by wearing a removable splint or by being “buddy strapped” to a non-injured finger next to the injured finger. The non-injured finger acts as a “moving splint” to support the injured finger.
You can usually begin gentle hand exercises after 3 weeks.
Some hand fractures require surgery to realign and stabilize the fracture fragments. Surgery is often necessary for open fractures in which pieces of bone have broken through the skin.
Your doctor may need to make an incision to help reposition the bone fragments into their normal alignment. Small metal devices — such as wires, screws, pins, staples, and plates — may be used to hold the pieces of fractured bone in place.
After surgery, you may have to wear a splint or cast for a period of time to protect the fracture. If the bone changes position during healing, your finger may lose some function. Your doctor will talk with you about when it is safe to begin range-of-motion exercises and to resume your normal activities after surgery.
Because some fractures require prolonged immobilization in a cast or splint, your hand and fingers may become stiff. Your doctor or, in some cases, an occupational therapist, physical therapist or hand therapist, will provide specific exercises to help decrease stiffness and improve function.
Even after carefully following therapy instructions after fracture treatment, some patients may continue to have difficulty with stiffness or a contracture (loss of motion) in the hand. If this occurs, your doctor may recommend a surgical procedure to help restore motion and/or function to your finger. Commonly used procedures include:
Generally, these procedures are used once a fracture has healed and there is no evidence of progress or improvement in the return of function to the injured finger. Your doctor will talk with you about whether you need an additional procedure and, if so, how it may affect your recovery.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec