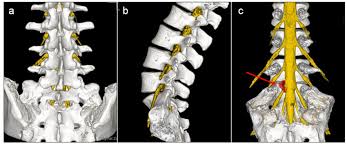
Spinal fusion is a surgical procedure designed to join two or more vertebrae in the spine, eliminating motion between them. This technique is commonly used to stabilize the spine, relieve pain, and correct deformities. It is an important intervention for patients suffering from various spinal conditions that cause instability, chronic pain, or neurological symptoms. Understanding spinal fusion is essential for patients considering treatment options for spinal disorders, as well as for caregivers and healthcare professionals involved in spine care.
The human spine is a complex structure composed of 33 vertebrae stacked in a column, separated by intervertebral discs that act as shock absorbers. The spine is divided into cervical (neck), thoracic (mid-back), lumbar (lower back), sacral, and coccygeal regions. Each vertebra consists of a vertebral body anteriorly and a vertebral arch posteriorly, which protects the spinal cord running through the spinal canal.
The spine provides structural support, enables flexible movement, and protects the spinal cord and nerve roots. Intervertebral discs and facet joints allow for motion between vertebrae. When these structures are damaged or degenerate, abnormal motion or instability can occur, leading to pain and neurological symptoms.
Patients who may benefit from spinal fusion often present with:
Symptoms vary depending on the underlying condition and the spinal level involved.
Before considering surgery, conservative management is often attempted:
When conservative treatments fail or when instability or neurological compromise is severe, spinal fusion surgery may be recommended.
Spinal fusion involves several key steps:
The goal is to create a solid bony bridge between vertebrae, eliminating motion and stabilizing the spine.
Recovery after spinal fusion involves:
Complete fusion may take several months, during which adherence to rehabilitation protocols is crucial.
As with any surgery, spinal fusion carries potential risks:
Discussing risks with a surgeon helps patients make informed decisions.
Most patients experience significant pain relief and improved stability after spinal fusion. Success rates vary depending on the underlying condition, patient health, and adherence to postoperative care. Fusion typically results in reduced motion at the operated segment but may increase stress on adjacent levels. Long-term outcomes are generally favorable when surgery is appropriately indicated.
Spinal fusion is a vital surgical option for treating spinal instability, deformities, and nerve compression. Understanding the anatomy, causes, symptoms, and treatment options empowers patients to make informed decisions. While non-surgical treatments are first-line, spinal fusion offers relief when conservative measures fail. Careful surgical planning, postoperative rehabilitation, and awareness of risks contribute to successful outcomes. If you or a loved one are experiencing significant spinal symptoms, consult a healthcare professional to explore the best treatment approach tailored to your needs.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec