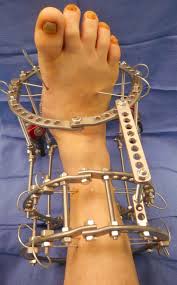
External Fixation is a surgical technique used to stabilize broken bones using an external frame attached to the bone with pins, wires, or screws. Unlike internal fixation (which uses plates, screws, or rods placed inside the body), external fixation provides stability from outside the skin. It is commonly used in severe fractures, open injuries, or situations where internal fixation is not immediately possible due to infection, swelling, or patient condition.
This technique plays a crucial role in trauma management, complex fractures, limb reconstruction, and even in correcting bone deformities. External fixation not only stabilizes bones but also allows surgeons to manage soft tissue injuries simultaneously.
Bones form the structural framework of the body, enabling movement, supporting weight, and protecting vital organs. When a bone fractures, proper alignment and stability are essential for healing.
Bone healing process involves inflammation, callus formation, and remodeling.
Stability is vital—too much movement at the fracture site can delay healing.
Soft tissue integrity (muscles, skin, nerves, vessels) influences surgical decision-making.
External fixation is particularly useful when soft tissue is severely damaged, as it allows access for wound care without disturbing fracture stabilization.
External fixation is often used in cases where fractures are complex, unstable, or associated with significant soft tissue damage. Common causes include:
High-energy trauma: Road traffic accidents, industrial injuries, or falls from height.
Open fractures: When the bone pierces the skin, raising infection risk.
Severe soft tissue injuries: Where swelling or wounds make internal fixation unsafe.
Infected fractures (osteomyelitis): External fixation avoids placing foreign material inside infected bone.
Complex or multi-fragmented fractures: Especially in long bones (femur, tibia, humerus).
Corrective procedures: For limb lengthening, deformity correction, or joint fusion.
Patients with poor bone quality, systemic infection, or severe trauma are more likely to need external fixation.
The typical signs and symptoms of fractures that may require external fixation include:
Severe localized pain at the injury site.
Visible deformity or abnormal limb angulation.
Swelling, bruising, or bleeding (in open fractures).
Inability to move or bear weight.
Exposed bone fragments in open fractures.
Associated soft tissue injuries such as lacerations or crush wounds.
In some cases, patients may present with shock due to blood loss, especially with high-energy trauma.
Diagnosis of fractures requiring external fixation involves:
Clinical Examination
Inspection for deformity, wounds, or exposed bone.
Palpation for tenderness, crepitus, or instability.
Assessment of circulation (pulses, capillary refill) and nerve function.
Imaging Studies
X-rays: Standard imaging to identify fracture type and displacement.
CT scans: Useful for complex or joint-involving fractures.
MRI: Helpful for assessing associated ligament, tendon, or soft tissue injuries.
Laboratory Tests
Preoperative investigations (blood counts, infection markers, coagulation profile).
Accurate diagnosis ensures appropriate surgical planning.
Casting or splinting for stable fractures.
Traction in selected long-bone fractures.
Pain control, rest, and physiotherapy.
Internal fixation: Plates, screws, or rods for definitive fixation.
External fixation: Chosen when internal fixation is unsafe or impractical.
Hybrid fixation: A combination of external and internal devices in complex cases.
External fixation is often a temporary measure in trauma settings, later replaced by internal fixation once the soft tissue heals. However, in some cases (like infected fractures or deformity correction), it serves as definitive treatment.
The steps in an external fixation procedure generally include:
Anesthesia: General or regional anesthesia is administered.
Preparation: The injured area is cleaned and sterilized.
Pin or wire insertion: Metal pins or wires are drilled into the bone above and below the fracture site through small skin incisions.
Frame application: The pins are connected to an external frame (bars, rings, or rods). This stabilizes the bone fragments.
Fracture alignment: The surgeon adjusts the frame to achieve proper alignment.
Wound management: In open fractures, wound care or skin grafting may be performed.
Closure: Dressings are applied around pin sites, and the patient is shifted to recovery.
The type of external fixator (uniplanar, biplanar, circular/Ilizarov) depends on the fracture’s complexity.
Recovery and rehabilitation after external fixation involve:
Hospital stay: Monitoring for infection, pain control, and wound care.
Pin site care: Daily cleaning of pin insertion sites to prevent infection.
Physiotherapy: Early mobilization of adjacent joints to prevent stiffness.
Weight-bearing: Depending on the fracture and fixator, partial or full weight-bearing may be allowed.
Nutrition: Adequate intake of protein, calcium, and vitamin D supports healing.
Follow-up visits: Regular X-rays to monitor bone healing and frame stability.
The fixator is typically removed once the bone has healed sufficiently, usually after several weeks to months.
Potential complications of external fixation include:
Pin site infection (most common).
Neurovascular injury during pin insertion.
Delayed union or nonunion (bone fails to heal properly).
Malunion (bone heals in incorrect position).
Joint stiffness due to prolonged immobilization.
Hardware-related issues: Loose or broken pins, frame instability.
Scarring or cosmetic concerns.
Prompt management of complications ensures better outcomes.
The prognosis after external fixation depends on the severity of the injury and associated soft tissue damage.
Most patients regain functional use of the limb once the fracture heals.
In cases of severe trauma, staged surgeries (external fixation followed by internal fixation) improve results.
With proper care, pin site infections are manageable and rarely lead to serious complications.
Patients undergoing limb reconstruction or deformity correction can achieve excellent long-term outcomes with patience and rehabilitation.
Seek medical attention immediately if you experience:
Sudden severe pain or swelling after an injury.
Visible deformity or exposed bone.
Inability to move or bear weight on a limb.
Signs of infection at pin sites (redness, pus, fever).
Loosening or displacement of the external fixator frame.
Prompt consultation ensures timely treatment and avoids long-term disability.
External fixation is a vital orthopedic technique for stabilizing complex fractures, especially when soft tissue injuries or infection make internal fixation unsuitable. By providing stability from outside the body, it allows both fracture healing and wound management. While the procedure carries risks such as infection and stiffness, careful postoperative care and rehabilitation usually lead to good functional recovery.
If you have sustained a serious injury or fracture, consult an orthopedic specialist promptly. Early intervention with the right treatment approach can make the difference between long-term disability and a successful recovery.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec