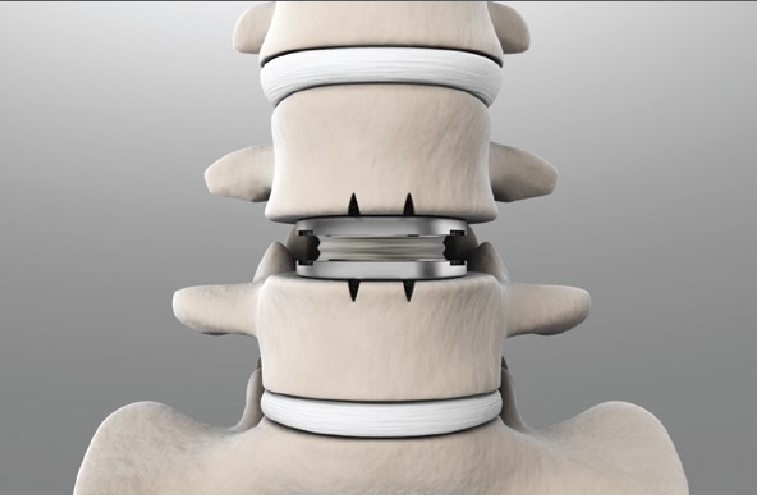
Cervical disc replacement (CDR) is a surgical procedure designed to treat degenerative disc disease or other cervical spine conditions that cause neck pain, arm pain, or neurological symptoms. Unlike traditional spinal fusion, which permanently joins two vertebrae, cervical disc replacement involves removing a damaged cervical disc and replacing it with an artificial disc. This procedure aims to preserve motion at the affected spinal segment, potentially reducing adjacent segment degeneration and improving overall neck function.
Cervical disc replacement is important because it offers an alternative to fusion surgery, which can limit neck mobility and sometimes lead to further spinal problems. For patients suffering from chronic neck pain or nerve compression due to disc degeneration, CDR can provide significant pain relief and functional improvement.
The cervical spine consists of seven vertebrae (C1 to C7) stacked one on top of another, separated by intervertebral discs. These discs act as shock absorbers and allow flexibility and movement of the neck. Each disc has a tough outer layer called the annulus fibrosus and a gel-like center called the nucleus pulposus.
Nerves exit the spinal cord through openings between the vertebrae called foramina. When a cervical disc degenerates, herniates, or collapses, it can compress these nerves or the spinal cord itself, leading to pain, numbness, or weakness in the neck, shoulders, arms, or hands.
Patients with cervical disc problems often present with:
Symptoms typically worsen with neck movement and may improve with rest.
Diagnosing cervical disc problems involves a combination of clinical evaluation and imaging studies:
Initial management often involves conservative measures:
When conservative treatments fail or neurological symptoms worsen, surgery may be indicated. Options include:
CDR is preferred in selected patients to maintain neck mobility and reduce stress on adjacent segments.
Cervical disc replacement is typically performed under general anesthesia and involves the following steps:
The procedure usually takes 1 to 2 hours, and patients may stay in the hospital for 1 to 2 days.
Recovery after cervical disc replacement involves:
Most patients return to normal activities within 4 to 6 weeks, with full recovery taking several months.
While cervical disc replacement is generally safe, potential risks include:
Discussing risks with a spine surgeon is essential before surgery.
Cervical disc replacement has shown favorable outcomes in appropriately selected patients:
Long-term studies indicate durable results, but ongoing follow-up is important to monitor implant integrity.
Cervical disc replacement is an advanced surgical option for treating cervical disc degeneration and related nerve compression. By preserving motion and reducing stress on adjacent spinal segments, it offers significant benefits over traditional fusion surgery for many patients. Understanding the anatomy, causes, symptoms, and treatment options can help individuals make informed decisions about their care. If you experience persistent neck pain or neurological symptoms, consult a qualified healthcare professional to explore the best treatment approach tailored to your needs.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec