Parathyroid hormone (PTH) is a critical regulator of calcium and phosphate metabolism in the human body. Secreted by the parathyroid glands, PTH plays a vital role in maintaining stable blood calcium levels, which are essential for numerous physiological processes including bone health, muscle function, nerve conduction, and blood clotting. Dysregulation of PTH secretion can lead to significant clinical conditions such as hyperparathyroidism or hypoparathyroidism, impacting overall health and quality of life. Understanding PTH’s function, causes of its imbalance, clinical presentation, and treatment options is essential for both healthcare professionals and patients.
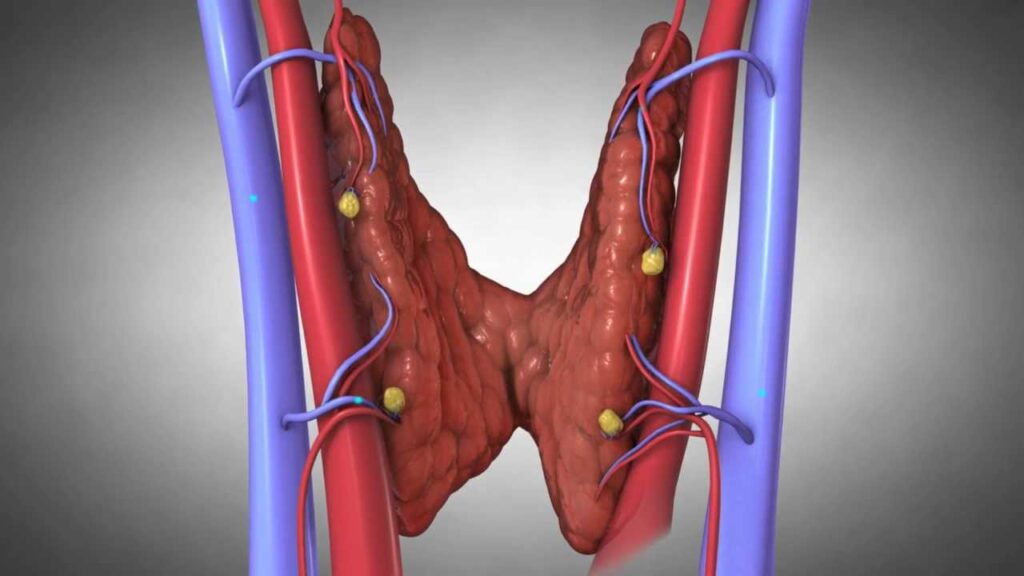
The parathyroid glands are four small, pea-sized endocrine glands located on the posterior surface of the thyroid gland in the neck. Despite their proximity to the thyroid, they have a distinct function: producing and secreting parathyroid hormone. PTH acts primarily on three target organs:
Together, these actions maintain serum calcium within a narrow physiological range, typically between 8.5 and 10.5 mg/dL.
Diagnosis involves a combination of clinical evaluation and laboratory investigations:
Parathyroidectomy involves the surgical removal of one or more parathyroid glands:
Minimally invasive techniques may be used depending on localization and surgeon expertise.
Parathyroid hormone is essential for calcium homeostasis and overall metabolic balance. Disorders of PTH secretion, whether excess or deficiency, can lead to significant health issues but are often manageable with timely diagnosis and appropriate treatment. If you experience symptoms suggestive of parathyroid dysfunction or have risk factors, consulting a healthcare professional is crucial. Advances in medical and surgical therapies continue to improve prognosis and quality of life for affected individuals.
Aenean porta orci nam commodo felis hac ridiculus fusce fames maximus erat sed dictumst blandit arcu suspendisse sollicitudin luctus in nec